
Learn how an integrated PBM solution helps insurance executive Aaron boost in-network penetration from 72% to 85% ― saving $1.3 million ― within six months.
Keeping transactions in-network leads to lower costs, better clinical oversight and claimant care.
Meet AARON

Aaron runs the workers’ compensation division of a large insurance company. His responsibilities include managing his customers’ spend and ensuring the care that claimants receive is appropriate for their injuries. After meeting with his current Pharmacy Benefit Manager (PBM), he decided not to renew his contract but instead open it up to bids. While they had provided adequate service, Aaron felt they just weren’t producing the expected level of cost savings.
Time for a change
Among other PBMs, Aaron invited Optum, a leading workers’ compensation PBM, to respond to his company’s RFP. Optum was able to run a Pharmacy Physical, which analyzed data from his current book of business in order to find gaps in cost containment. From this analysis, Optum quickly determined too many of his company’s transactions were being run out of network and that there was a considerable opportunity for savings by switching to Optum and its proprietary Tmesys® network of nearly 70,000 contracted pharmacies – from national chains to independent stores.
Keeping transactions in network
The Optum PBM solution offers two pharmacy services options: a Retail Pharmacy Program and a Home Delivery Program for the ultimate in convenience.
The Optum retail solution is built on best-in-class foundational programs that ensure transactions are captured in network. Claimants not using a contracted pharmacy, or not presenting their pharmacy card for their work-related injury, can cause the transactions to be taken out of network. Because Optum owns and manages SRPS, the industry’s largest third-party biller, those transactions are automatically redirected back into the Optum network at point of sale. As a result, Optum is able to deliver network penetration rates of up to 98%.
With transactions processing in network, Optum applies unique business rules, custom drug utilization review parameters and network discounts at the point of sale. This added layer of protection ensures that the claimant receives the right medication at the right time, clinical oversight is applied and paper bills are eliminated. Here’s how the Optum network enforcement works:
- A real-time eligibility match is performed on all transactions.
- Eligible transactions are electronically re-indexed to Optum.
- The dispensing pharmacy is notified of the Optum BIN, which allows the transaction
to process. - In-network rates, medication plans and point-of-sale edits are applied on the transaction.
The Optum innovative First Fill® and Samaritan Dose programs also help claimants receive medications promptly while keeping transactions in network.
As a final layer of protection, the Optum network also allowed Aaron to capture occupational health clinics, physician-dispensing locations, and specialty and compounding facilities as in network, which are typically received as out-of-network transactions.
Optum delivered savings
Aaron partnered with Optum for his PBM business and immediately saw a spike in savings. Within six months, his in-network penetration went from 72% to 85%, which equated to $1.3 million in savings. Plus, once he converts to Optum home delivery, his projected in-network penetration rate is expected to reach between 95-98% by the end of year two.
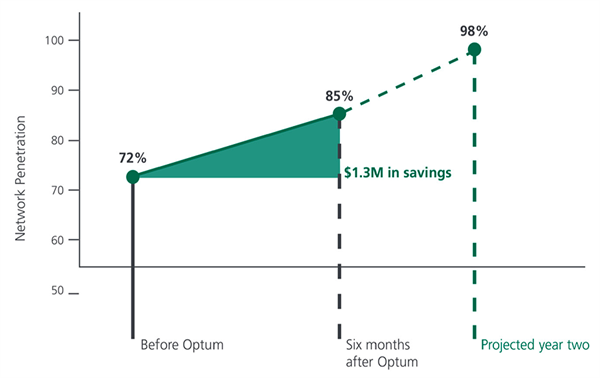
Results
Aaron is happy he made the switch and partnered with Optum. He knows he is saving a substantial amount of money, not only for his business but also for his clients. Plus, the increased in-network penetration allows for better clinical oversight, which leads to better care and a better quality of life for all his claimants.